When you think of endometriosis symptoms, painful periods probably come to mind. But for many people, the pain doesn't stop once menstruation ends. In fact, endometriosis and painful ovulation are closely linked, and ovulation can be just as uncomfortable, or in some cases, even more distressing, than period pain.
If you experience sharp, aching, or cramping pain mid menstrual cycle (around the time when you're ovulating), you're likely wondering whether it's normal or not, where it should be felt, and whether endometriosis affects ovulation itself.
The short answer is that endometriosis can change how ovulation feels, where pain is located, and how intense it becomes. In this article, you'll learn how ovulation and endometriosis pain are linked, and why endo symptoms are often dismissed, misdiagnosed, or misunderstood.
Quick Summary: Endometriosis and Ovulation Pain
- Endometriosis and painful ovulation are commonly linked.
- Ovulation and endometriosis pain can feel sharp, burning, or deep in the pelvis.
- Where ovulation pain is located often depends on lesion placement.
- Severe pain with endometriosis mid-cycle is not normal.
- Inflammation and nerve sensitization are key drivers.
- Anti-inflammatory support, including NAC, may help reduce flare intensity.
In this article:
- What Is Ovulation Pain? (And Where Is Ovulation Pain Located?)
- Ovulation Pain Symptoms in Endometriosis: What Mid-Cycle Flares Feel Like
- Does Endometriosis Affect Ovulation? Here’s What Happens to the Ovaries
- Ovulation and Endometriosis Pain vs. Period Endometriosis Pain
- Why Severe Pain With Endometriosis at Ovulation Is Often Dismissed
- When to Seek Support (And Remedies That Can Help))
- How to Treat Endometriosis and Painful Ovulation
- When Ovulation Pain Is an Emergency
- The Bottom Line on Endometriosis & Ovulation Pain
- FAQ: Endometriosis and Painful Ovulation
What Is Ovulation Pain? (And Where Is Ovulation Pain Located?)
Ovulation pain, sometimes called mittelschmerz (German for “middle pain”), refers to discomfort that occurs when an ovary releases an egg.
For some, ovulation pain is mild and fleeting or barely noticeable at all. But for others, especially those with endometriosis, it can be intense and disruptive.
While most studies focus on endo pain related to menstruation, some have found that in the general population, up to 40% of people experience ovulation pain1 (or some type of discomfort) at some point in their cycle, and usually it's mild and short-lived.
That means that if you regularly experience mid-cycle pain that is severe, prolonged, or debilitating, it's not typical for normal ovulation—and it may warrant an evaluation for underlying conditions, including endometriosis.
Related:
Pain During Ovulation: Is It Normal?
Ovulation Signs: How Do I Know If I’m Ovulating?
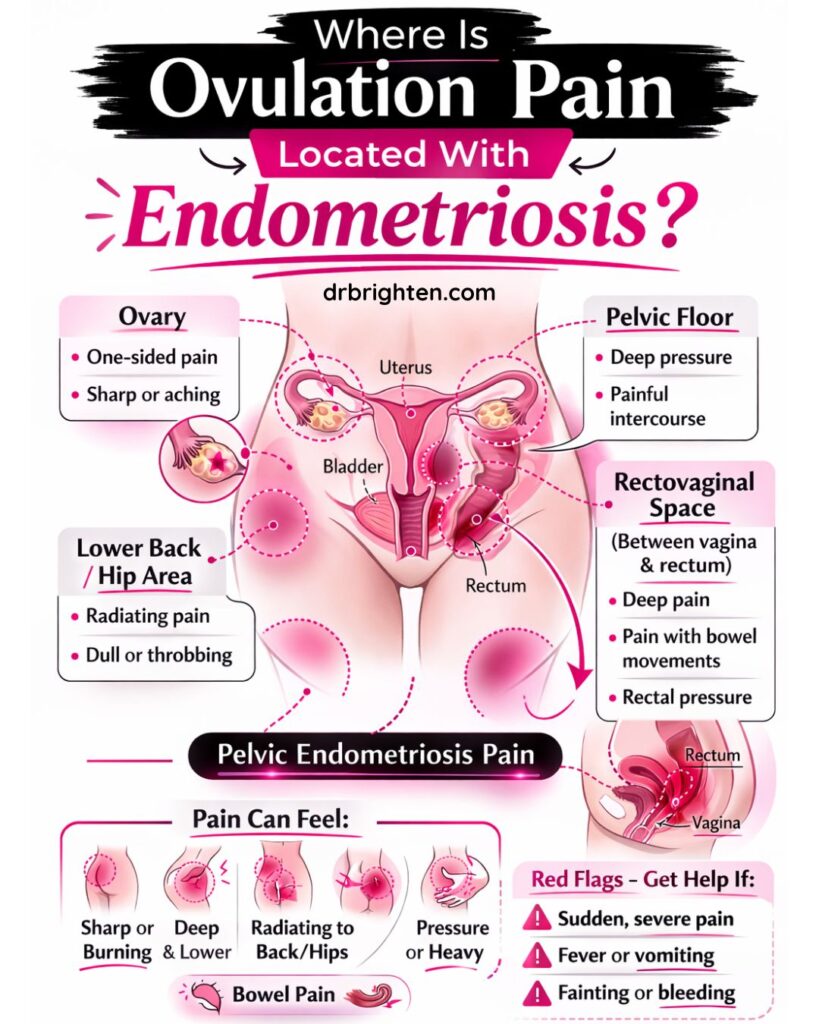
Where Is Ovulation Pain Located With Endometriosis?
In terms of where ovulation pain is located, it's most commonly felt:
- On one side of the lower abdomen (depending on which ovary ovulates)
- Deep in the pelvis
- In the lower back or hips
- Occasionally radiating into the thighs or butt area (rectum)
As mentioned above, with endometriosis, this pain isn't always localized to the ovaries, meaning you can feel it spreading outward. That can be due to adhesions2, inflammation, and nerve involvement, which can cause pelvic endometriosis pain that affects the lower body beyond the ovary itself.
If Ovulation Pain Is Becoming Severe
If you experience:
- Mid-cycle pain that worsens each month
- Severe pain with endometriosis that disrupts life
- Ovulation symptoms with endometriosis that include bowel or bladder pain
You may benefit from:
Anti-inflammatory nutrition
- Targeted antioxidant support (such as NAC)
- Hormonal evaluation
- Pelvic floor therapy
Learn more about evidence-based supplements for endometriosis here.
Endometriosis and Painful Ovulation: Why Ovulation Triggers Pelvic Endometriosis Pain
Endometriosis occurs when tissue similar to the uterine lining grows outside the uterus. Tissue can grow on the ovaries, pelvic walls, bowel, bladder, or behind the uterus. This tissue responds to hormonal changes during the cycle, including ovulation, when there's a peak in luteinizing hormone (LH)3 and estrogen.
Endometriosis is associated with chronic pelvic pain in up to roughly 80% of those affected4, and ovulation can be one of the times when this pain flares due to heightened inflammation and sensitization of pelvic tissues.
During ovulation:
- Estrogen peaks
- LH surge causes the ovary to swell slightly
- Inflammatory chemicals are released to release the egg from the ovary
- Fluid and blood can potentially irritate surrounding tissues
In someone with endometriosis, these normal processes interact with inflamed, sensitized tissue5. This is why if you have endometriosis, ovulation pain symptoms can feel sharp, burning, stabbing6, or deeply cramp-like.
This also explains why cramps during ovulation in those with endometriosis can sometimes be mistaken for digestive or musculoskeletal issues, such as IBS, constipation, gas pain, hip flexor strain, or lower back dysfunction. Many of these digestive issues are common endometriosis symptoms, especially mid-cycle or during menstruation.
Related: What Causes Endometriosis & Natural Treatments That Help
Ovulation Pain Symptoms in Endometriosis: What Mid-Cycle Flares Feel Like
Ovulation doesn't always or only cause painful sensations. It can also trigger digestive issues, such as bloating, for example, or other types of sensations that aren't necessarily uncomfortable but still noticeable.
Ovulation symptoms7 with endometriosis can include:
- One-sided pelvic pain that lasts for hours or even 1-2 days (ovulation pain may be more intense on the side where endometriosis lesions or ovarian cysts are present, and it can switch sides month to month depending on which ovary releases an egg)
- Cramping similar to period pain
- Pain during bowel movements
- Mild vaginal bleeding
- Pain with movement or exercise
- Bloating or pressure in the lower abdomen
- Nausea and loss of appetite
- Fatigue
- Pain with intercourse around ovulation
For some, this pain escalates into severe discomfort that's intense enough to interfere with daily life, such as making it difficult to work, exercise, or sleep.
If you develop severe pain with endometriosis, talk to your healthcare provider about what you can do to manage your symptoms rather than trying to “tough it out.” Your provider might decide to do tests8 such as a blood test, X-rays, a pelvic ultrasound, or a computed tomography (CT) scan to determine what's causing your pain and how to treat it.
Does Endometriosis Affect Ovulation? Here’s What Happens to the Ovaries
Aside from being uncomfortable, you might wonder, does endometriosis affect ovulation itself—for example, by delaying it or causing anovulatory cycles (when ovulation doesn't occur).
Ovulation can still occur regularly even if you have endometriosis. But that said, endo can potentially:
- Alter ovarian function
- Increase inflammation around the ovaries
- Cause ovarian cysts (called endometriomas)
- Disrupt follicle development in some cases
This doesn't mean that ovulation always stops when you have endo, but it can become more painful, less predictable, or associated with fertility challenges for some people.
And because painful ovulation does not automatically mean ovulation isn’t occurring, it doesn't mean that pregnancy isn’t possible—but it can signal inflammation that deserves evaluation if you're trying to conceive.
If this sounds familiar, it’s important to track when the pain occurs across your cycle and bring that information to a clinician who understands endometriosis. Getting evaluated can help preserve ovulation, protect your fertility, and prevent pain from becoming more severe over time.
Related:
Getting Pregnant with Endometriosis
Ovulation and Endometriosis Pain vs. Period Endometriosis Pain
While period-endometriosis pain is widely recognized, ovulation pain is often overlooked. Yet both are driven by inflammation, nerve involvement, and hormonal signaling9—all of which can worsen over time if they're not addressed.
Here are some of the key differences between endo pain caused by ovulation versus periods (menstruation):
Period endometriosis pain:
This is primarily driven by uterine contractions and the inflammatory response to menstrual shedding.
In endometriosis, tissue similar to the uterine lining also responds to hormonal signals outside the uterus, which means inflammation and pain can extend beyond the uterus itself. This is why pelvic endometriosis pain often radiates to the lower back, hips, or thighs during menstruation.
Ovulation pain:
On the other hand, this type of pain occurs mid-cycle and is linked to the rupture of the ovarian follicle, a sharp rise in estrogen, and localized fluid release into the pelvis.
For someone without endometriosis, this might cause mild or brief discomfort10 for several hours to one day. But with endometriosis, ovulation can trigger a disproportionate inflammatory response, especially if lesions or scar tissue are present on or near the ovaries, pelvic ligaments, or surrounding nerves.
Both types of pain:
In endometriosis, both phases can be painful because the condition is progressive and inflammatory.
When endo isn't treated, scar tissue can accumulate, adhesions can restrict normal organ movement, and nerves can become increasingly sensitized. This lowers the body’s pain threshold and makes sensations that were once tolerable feel intense or even debilitating.
This process is known as central sensitization, where the nervous system becomes hyper-reactive and amplifies pain signals. As a result, ovulation and period pain may feel sharper, last longer, or spread to other areas of the body, even when visible disease activity appears minimal.
Why Severe Pain With Endometriosis at Ovulation Is Often Dismissed
Endometriosis is now understood as a systemic inflammatory condition, not just a gynecologic one. Research shows inflammation from endometriosis can affect the immune system, nervous system, and even brain signaling.
However, endometriosis pain is often still dismissed because menstrual pain has been incorrectly normalized. Yet, progressive, cyclic pain is not typical and should never be minimized.
Endometriosis can take years to diagnose, in some cases, for several reasons:
- Symptoms overlap with IBS, bladder issues, or anxiety
- Imaging tests often fail to detect lesions
- Pain outside menstruation is not taken seriously
- Ovulation pain is labeled as “normal” and is only mild
Yet ovulation and endometriosis pain that worsens over time is a major red flag. Pain that is cyclic, progressive, and pelvic in nature deserves deeper evaluation.
Related: Endometriosis and IBS: Symptom Connection and Solutions
Does Endometriosis Go Away After Menopause? (And What Happens to Ovulation Pain?)
While some women do experience symptom relief after menopause, others continue to struggle with endometriosis after menopause. In some cases, endo symptoms after menopause can even get worse during the transition due to persistent inflammation.
Endo lesions can persist (and remain active) even after hormone levels drop (such as progesterone), continuing to cause discomfort. And endo pain, along with other symptoms like “endo belly” bloating, can continue post-menopause, especially when endometriosis affects the bladder, bowel, or other organs.
Related: Does Endometriosis Go Away After Menopause? Here's the Truth
When to Seek Support (And Remedies That Can Help))
If you experience the symptoms below, these patterns point toward endometriosis rather than isolated ovulation discomfort:
- Persistent ovulation pain mid-cycle
- Worsening pelvic endometriosis pain
- Cramping mid-cycle
- Pain that interferes with daily life
- Both ovulation and period pain occur in most months/cycles
How to Treat Endometriosis and Painful Ovulation
While there's no permanent cure for endo, there are ways to lower pain, all of which are aimed at reducing inflammation, limiting lesion activity, and calming an over-sensitized nervous system. This can include options like:
Pelvic floor physical therapy:
Chronic pelvic pain often causes the pelvic floor muscles to become tight, guarded, or dysfunctional, which can amplify pain signals. Pelvic floor physical therapy works to release tension, improve coordination, and retrain muscles to reduce pain during ovulation, menstruation, and daily movement.
Using birth control pills:
Hormonal birth control works by preventing ovulation, which for some people, can help ovulation related pain. But it is important to note that birth control pill do not stop lesion progression.
Targeted hormonal therapies:
These therapies, such as progestins or other hormone-modulating medications, aim to slow the growth and activity of endometriosis lesions. By altering estrogen signaling, they can help reduce inflammation and pain progression, though they may come with side effects that require careful monitoring.
Anti-inflammatory nutrition:
An anti-inflammatory diet focuses on stabilizing blood sugar and reducing inflammatory triggers that worsen pelvic pain, including ultra-processed foods and excess sugar. Emphasizing omega-3 fats, fiber-rich plants, and antioxidant-rich foods—especially foods high in polyphenols—can help calm systemic inflammation.
Best Supplements for Endometriosis and Painful Ovulation
Certain supplements may help support pain management and inflammation control in endometriosis, especially when used alongside anti-inflammatory nutrition. While supplements are not considered a treatment for endometriosis, they can be a helpful adjunct therapy.
- A magnesium supplement, such as magnesium glycinate (found in Magnesium Plus), is often helpful for relaxing smooth muscle, easing pelvic cramping, and supporting nervous system regulation without causing digestive upset.
- Omega-3 fatty acids, which you'll find in Omega Plus, can reduce inflammatory signaling linked to endometriosis-related pain.
- Curcumin, the active ingredient in turmeric, supports inflammatory pathway balance.
- Vitamin D (especially D3, found in my Vitamin D3/K2 drops) assists in immune regulation and pain perception.
- B vitamins, particularly vitamin B1 (thiamine), B6, B12, and folate, which are all found in B-Active Plus, support nerve function, energy production, and pain signaling, which can help manage endometriosis-related pain and fatigue. Vitamin B6 may also support prostaglandin balance, while B12 and folate play roles in nervous system health and inflammation regulation.
NAC for Endometriosis and Ovulation Pain: What the Research Shows
Endometriosis is not just a hormonal condition — it is an inflammatory and oxidative stress–driven disease. That distinction matters when we talk about why ovulation can be so painful and what may actually help.
One of the most studied antioxidant compounds in endometriosis research is N-acetylcysteine (NAC).
How NAC Works in the Body
NAC is a precursor to glutathione, one of the body’s most powerful antioxidants. Glutathione plays a central role in:
- Neutralizing oxidative stress
- Regulating immune signaling
- Supporting liver detoxification pathways
- Protecting ovarian tissue
By increasing glutathione availability, NAC may help reduce the inflammatory signaling that contributes to both period endometriosis pain and ovulation-related pelvic pain.
What Research Says About NAC and Endometriosis
Several clinical studies have explored NAC’s role in endometriosis management. Research has shown that NAC may:
- Reduce the size of endometriomas (ovarian cysts associated with endometriosis)
- Lower inflammatory markers
- Improve pelvic pain symptoms
- Support ovulatory function in some individuals
In one well-known study, women taking NAC experienced reductions in cyst size and, in some cases, avoided planned surgery. While NAC is not a cure for endometriosis, these findings suggest it may play a supportive role in reducing lesion activity and inflammatory burden.
Because oxidative stress is also linked to egg quality and ovarian health, NAC is sometimes used in fertility-support protocols for individuals with endometriosis.
Can NAC Help Ovulation Pain Specifically?
Ovulation pain in endometriosis is driven by a combination of:
- Local inflammation
- Fluid release into the pelvis
- Activated immune cells
- Sensitized nerves
Since NAC helps regulate oxidative stress and inflammatory cytokines, it may help reduce the intensity of mid-cycle pain flares. Many clinicians use NAC as part of an anti-inflammatory strategy to support individuals experiencing cramps during ovulation with endometriosis.
That said, NAC works best as part of a comprehensive plan that includes anti-inflammatory nutrition, hormonal evaluation, and nervous system support.
Choosing a High-Quality NAC Supplement
When selecting NAC, quality and dosing matter. Therapeutic research protocols typically use clinically relevant doses divided throughout the day to maintain stable antioxidant support.
Dr. Brighten Essentials NAC is formulated to provide evidence-aligned dosing designed to support antioxidant defenses, inflammatory balance, and ovarian health. It can be used alongside magnesium, omega-3 fatty acids, and other targeted nutrients as part of a personalized endometriosis support plan.
Individualized pain-management strategies:
Because endometriosis pain is complex and often involves nerve sensitization, pain management needs to be personalized rather than one-size-fits-all. This can include nervous system support, lifestyle adjustments, supplements, or other integrative therapies.
Related:
19 Ways to Find Endometriosis Relief Naturally
Best Supplements for Endometriosis (Evidence-Based Guide)
When Ovulation Pain Is an Emergency
Mild mid-cycle discomfort can be normal. Severe, sudden, or unusual pain is not.
While endometriosis and painful ovulation are closely linked, not all pelvic pain during ovulation should be assumed to be “just endo.” Certain symptoms require urgent medical evaluation.
Seek immediate medical care if ovulation pain is accompanied by:
- Sudden, severe abdominal pain that feels different from your usual pattern
- Fainting or feeling like you might pass out
- Fever or chills
- Persistent vomiting
- A rigid or extremely tender abdomen
- Heavy vaginal bleeding
- Pain that rapidly worsens over hours
These symptoms may indicate:
- Ovarian torsion (twisting of the ovary)
- A ruptured ovarian cyst with internal bleeding
- An ectopic pregnancy
- Pelvic infection
- Appendicitis
These conditions can mimic ovulation and endometriosis pain but require urgent evaluation and sometimes surgical intervention.
How to Tell the Difference Between Typical Ovulation Pain and an Emergency
Ovulation pain with endometriosis is usually:
- Cyclic (happens around the same time each month)
- One-sided
- Predictable in pattern
- Lasting hours to a couple of days
- Similar in character to prior flares
Emergency pain is often:
- Sudden and severe
- Different from your usual pattern
- Associated with systemic symptoms (fever, dizziness, nausea that won’t stop)
- Progressively worsening
If something feels significantly different from your baseline, it deserves attention.
Trust the Pattern — But Also Trust Your Instincts
Endometriosis pain is often dismissed. Many people are conditioned to normalize suffering. But new, escalating, or severe pain is information.
Even if you have confirmed endometriosis, do not automatically assume all pelvic pain is caused by it. Coexisting conditions are common.
If you are unsure, it is always appropriate to seek evaluation. Emergency clinicians can rule out life-threatening causes before attributing pain to ovulation or endometriosis.
Ovulation and endometriosis pain can be intense — but it should still follow a recognizable pattern.
Pain that is sudden, severe, accompanied by systemic symptoms, or dramatically different from your norm is not something to “wait out.”
When in doubt, get checked.
The Bottom Line on Endometriosis & Ovulation Pain
- Endometriosis and painful ovulation are closely connected, even though ovulation pain is rarely discussed.
- For those with endo, ovulation can trigger inflammation, nerve activation, and deep pelvic pain that mirrors or sometimes even exceeds period pain.
- If you have endo, it helps to recognize where ovulation pain is located and what it feels like, which can help you track your cycle and symptoms and get better care.
- Pain that is cyclic, progressive, and disruptive is not normal, whether it happens during your period or at ovulation. It is information your body is offering, and it deserves to be taken seriously.

FAQ: Endometriosis and Painful Ovulation
Endometriosis and painful ovulation are closely linked due to inflammation, nerve sensitization, and lesion activity near the ovaries. Severe or worsening mid-cycle pelvic pain is not considered normal and may benefit from targeted anti-inflammatory and antioxidant support.
Yes. Endometriosis can cause painful ovulation, especially when lesions or scar tissue are located near the ovaries, pelvic ligaments, or surrounding nerves. Ovulation is a naturally inflammatory event, and in people with endometriosis, that inflammation can trigger a disproportionate pain response. This is why ovulation and endometriosis pain often feel sharp, burning, or deeply cramp-like rather than mild and brief.
For some people, yes. While period endometriosis pain is more widely recognized, ovulation pain can be just as intense—or even worse—especially if lesions are located near the ovary that releases the egg that month. Mid-cycle inflammation combined with nerve sensitization can make ovulation pain severe and disruptive.
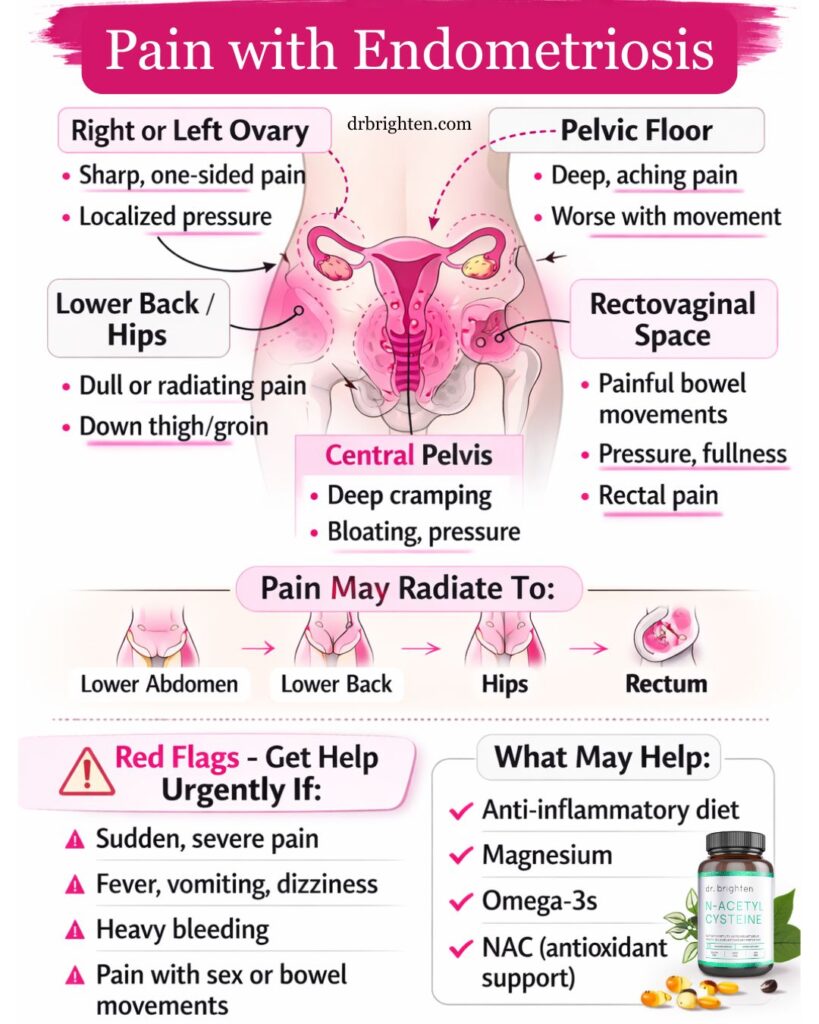
Ovulation pain with endometriosis is most commonly felt:
– On one side of the lower abdomen
– Deep in the pelvis
– In the lower back or hips
– Radiating into the thighs or rectal area
If adhesions or deep infiltrating lesions are present, pelvic endometriosis pain may spread beyond the ovary itself and feel more diffuse or widespread.
Typical ovulation discomfort lasts a few hours to one day. With endometriosis, ovulation pain can last 1–3 days and may feel progressively worse over time. Prolonged mid-cycle pain is not considered typical and should be evaluated, especially if it interferes with work, sleep, or daily functioning.
Endometriosis does not always stop ovulation, but it can affect ovarian function. Inflammation around the ovaries, endometriomas (ovarian cysts), and oxidative stress may:
– Disrupt follicle development
– Alter egg quality
– Make ovulation more painful
– Contribute to fertility challenges
Ovulation can still occur regularly, even when it is painful.
Yes, many people with endometriosis ovulate normally. However, ovulation may be more painful due to local inflammation and tissue sensitivity. Painful ovulation does not automatically mean ovulation has stopped, but it may signal underlying inflammation that deserves medical attention.
Ovulation involves a surge in luteinizing hormone (LH), a rise in estrogen, and the release of inflammatory mediators that allow the follicle to rupture. In someone with endometriosis, pelvic tissues are already inflamed and immune-activated. This amplified inflammatory environment can intensify pain during follicular rupture and fluid release.
Ovulation pain occurs mid-cycle and is triggered by follicle rupture and localized inflammation. Period endometriosis pain is driven by uterine contractions and inflammatory prostaglandins during menstrual shedding.
With endometriosis, both phases can be painful because lesions outside the uterus respond to hormonal shifts and activate surrounding nerves.
Mild cramping during ovulation can be normal in the general population. However, severe cramps during ovulation with endometriosis are not typical and often indicate lesion activity, adhesions, or nerve involvement. Persistent or worsening mid-cycle cramps should not be dismissed as “just ovulation.”
Yes. Ovulation pain may switch sides month to month because ovulation typically alternates between ovaries. However, if endometriosis lesions are concentrated on one side, pain may feel consistently worse on that side regardless of which ovary ovulates.
Ovulation pain may suggest endometriosis if it is:
– Severe or worsening over time
– Accompanied by bowel or bladder pain
– Associated with painful periods
– Causing fatigue, nausea, or bloating
– Interfering with daily life
Cyclic, progressive pelvic pain is a red flag and warrants further evaluation.
Yes. If lesions are located on the bowel or rectovaginal space, inflammation during ovulation can irritate those tissues and cause pain with bowel movements, rectal pressure, or bloating. This is sometimes misdiagnosed as IBS.
Not necessarily—but worsening or progressively longer pain can signal increasing inflammation, scar tissue formation, or central sensitization. Early evaluation and targeted treatment may help prevent escalation.
N-acetylcysteine (NAC) has been studied for its role in reducing oxidative stress and modulating inflammatory pathways associated with endometriosis. Research suggests NAC may help reduce lesion size, lower inflammatory cytokines, and support ovarian function.
Because ovulation is an inflammatory process, antioxidant support like NAC may help buffer the oxidative stress response during mid-cycle flares.
Endometriosis is driven by chronic inflammation and immune dysregulation. During ovulation, the body naturally releases inflammatory chemicals to facilitate egg release. In people with endometriosis, this inflammatory response is amplified, increasing pelvic endometriosis pain.
Reducing systemic inflammation is often a key part of managing both period and ovulation pain.
Seek medical evaluation if you experience:
– Severe pain with endometriosis mid-cycle
– Pain lasting more than 2–3 days
– Fever, vomiting, or fainting
– Sudden sharp pain unlike your usual symptoms
– Pain that disrupts daily activities
Persistent mid-cycle pain is not something you should “tough out.”
Yes. Inflammation, endometriomas, and oxidative stress may affect egg quality and ovarian reserve. However, many people with endometriosis conceive successfully. If you are trying to conceive and experiencing painful ovulation, early evaluation is important.
No. Ovulation pain can occur without endometriosis and is often mild and short-lived. Conditions such as ovarian cysts, pelvic infections, or gastrointestinal issues can also cause mid-cycle pain. The pattern, severity, and associated symptoms help differentiate causes.
References
- https://www.ncbi.nlm.nih.gov/sites/books/NBK549822/ ↩︎
- https://www.jci.org/articles/view/188787 ↩︎
- https://www.ncbi.nlm.nih.gov/sites/books/NBK549822/ ↩︎
- https://academic.oup.com/biolreprod/article/113/5/1029/8211700 ↩︎
- https://pubmed.ncbi.nlm.nih.gov/27048029/ ↩︎
- https://endometriosis.net/clinical/ovulation-pain ↩︎
- https://www.mayoclinic.org/diseases-conditions/mittelschmerz/symptoms-causes/syc-20375122 ↩︎
- https://www.health.harvard.edu/a_to_z/mid-menstrual-cycle-pain-mittelschmerz-a-to-z ↩︎
- https://my.clevelandclinic.org/health/diseases/9134-ovulation-pain-mittelschmerz ↩︎
- https://ufhealth.org/conditions-and-treatments/mittelschmerz ↩︎

