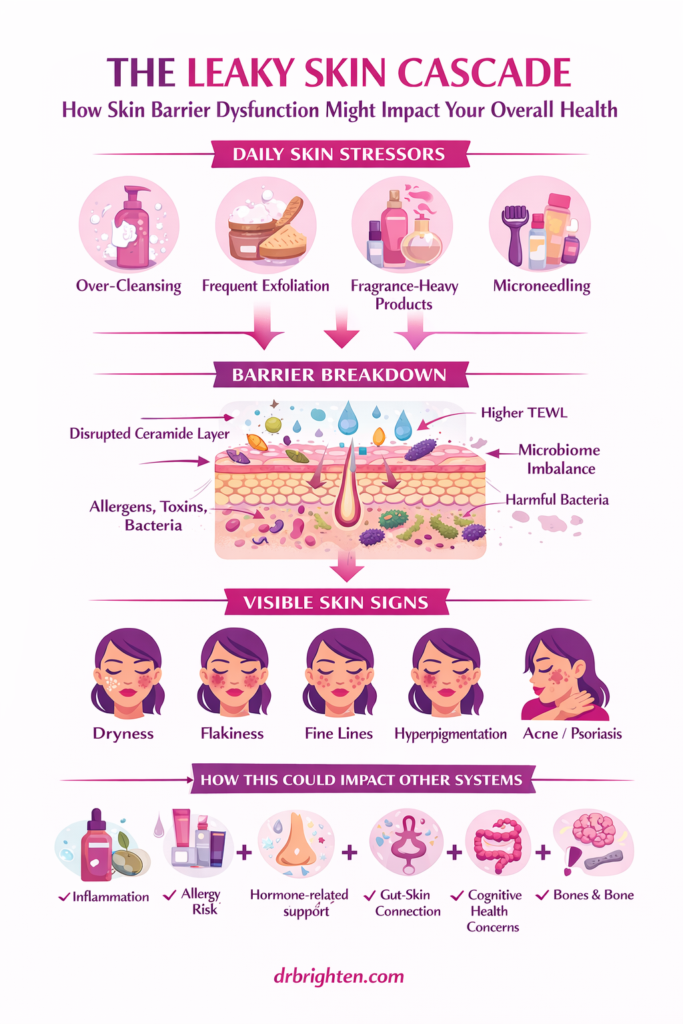
What if the condition of your skin was saying far more about your health than whether you need a new moisturizer? In this conversation, Dr. Jolene Brighten sits down with microbiologist Kiran Krishan to unpack a provocative idea: that skin barrier dysfunction may be linked not only to dryness, wrinkles, and hyperpigmentation, but also to systemic inflammation, hormone shifts, gut health, and even long-term disease risk.
This episode challenges the modern skincare mindset and asks a bigger question: are we trying to make skin look better while quietly making it less healthy?
What You’ll Learn in this Episode
In this episode, you’ll hear a deeper discussion about the skin as a living barrier, why the skin microbiome matters, and how everyday routines may be working against long-term skin health. Dr. Brighten and Kiran explore the intersection of skin aging treatment, women’s health, microbiome science, inflammation, and the gut-skin connection. They also discuss what “leaky skin” means, how to spot possible barrier dysfunction, and simple ways to rethink skincare through a more biologically informed lens.

Skin Microbiome: 12 Surprising Things You’ll learn in this Episode
- Why aged skin may be more than a cosmetic issue and could reflect deeper dysfunction in the body
- The startling claim that skin aging may be an independent risk factor for morbidity and mortality
- How barrier dysfunction on the face and neck may matter more than many people realize
- Why women may be more vulnerable to skin barrier damage because of daily product overload and procedures
- The difference between making skin look healthier and actually making it healthier
- What Kiran means by “leaky skin” and how it may relate to inflammation throughout the body
- The early signs of barrier dysfunction, including dryness, flakiness, fine lines, and hyperpigmentation
- Why hyperpigmentation is discussed as a marker of cellular stress and skin senescence
- The compelling statistic that children with dermatitis may have an eightfold higher risk of developing severe allergies
- How gut health, oral tolerance, and the immune system may influence skin symptoms in ways most people never hear about
- Why women with hormone shifts, acne, or PCOS-related inflammation may want to think differently about skin aging treatment
- The surprising acne data shared in the episode, including a reported 75% reduction in inflammatory and non-inflammatory lesions in a probiotic study discussed by Kiran
Skin Aging Treatment: Why the Conversation Needs to Change
One of the biggest themes in this episode is that the skin should not be treated like a surface to polish while ignoring its biology. Kiran argues that the skin is an organ and a barrier first. When that barrier is compromised, the result may be more than irritation or dryness. According to this discussion, barrier dysfunction may allow inflammatory triggers to penetrate deeper into the skin, activating immune responses that do not stay local.
That idea changes the conversation around skin aging treatment. Instead of asking only how to reduce fine lines or brighten the complexion, this episode asks whether those visible changes are signs that the barrier and the skin microbiome need support.
The Skin Barrier is Not just about Beauty
Throughout the episode, Dr. Brighten and Kiran return to the importance of the stratum corneum, the ceramide layer, and the role of resident microbes in maintaining skin health. When those systems are disrupted, the skin may lose moisture more easily and become more reactive.
The discussion suggests that what many people call normal aging may, in some cases, include accelerated dysfunction driven by inflammation, environmental exposures, microbiome disruption, and lifestyle patterns.
This is especially important for women, who are often encouraged to use more products, more treatments, and more aggressive routines.
The episode questions whether routines built around exfoliation, antimicrobial cleansing, microneedling, fragrance-heavy products, and long ingredient lists may do more harm than good for some people.
Signs Your Skin Barrier May Be Struggling
Kiran points to several clues that may suggest barrier dysfunction is developing:
- Skin that becomes very dry after washing
- Persistent flakiness
- Skin that feels increasingly thin
- Fine lines and wrinkles appearing earlier than expected
- Hyperpigmentation or “age spots” showing up earlier in life
- Skin that seems unable to hold moisture without constant topical support
The conversation also mentions trans epidermal water loss (TEWL) as a common way to measure how much water the skin is losing. In the context of this episode, that measurement is framed as a useful marker of barrier function.
Why the Microbiome Matters in Skin Aging Treatment
A key point in the episode is that the skin is not functioning alone. Beneficial microbes help maintain the skin’s environment, including its pH. Kiran explains that the skin ideally stays slightly acidic, and one reason is that microbes help break down oils and generate fatty acids that support that pH balance. When those microbes are repeatedly stripped away, the terrain of the skin may change in ways that make dysfunction more likely.
That is why this discussion pushes back on the idea that skin always needs to be “sterilized.” For many listeners, this will be one of the biggest mindset shifts in the episode. The guest suggests that in everyday life, many people may not need harsh cleansing or antimicrobial-heavy routines at all. Instead, they may benefit more from gentler cleansing, simpler ingredients, and allowing the skin to spend more time in a more natural state.
Hormones, Women’s Health, and the Skin Microbiome
This episode also brings women’s health into the center of the skin conversation. Hormones are discussed as major regulators of skin function, texture, hydration, and inflammation. The conversation touches on how hormone imbalance may contribute to skin changes and why some women may notice increased dryness, inflammation, or accelerated signs of aging during times of hormonal transition.
Dr. Brighten and Kiran also discuss PCOS, including cystic acne, systemic inflammation, and the possibility that gut dysfunction may amplify what happens at the skin level. In the episode, Kiran describes acne as something that may be influenced not only by sebum production and local inflammation, but also by gut-derived inflammatory triggers.
This makes the episode particularly relevant for women looking for a more root-cause-oriented approach to skin aging treatment. Rather than seeing skin changes as isolated, the conversation frames them as part of a bigger physiological picture involving hormones, immune balance, the gut, and barrier integrity.
The Gut-Skin Connection Comes into Focus
Another major topic is oral tolerance and the immune system. Kiran explains the idea that the body is built to encounter many antigens through the gut, where the immune system can learn not to overreact. When barrier dysfunction allows substances to enter through the skin instead, that process may unfold differently and potentially more inflammatory.
This framework is used to explain the “atopic march,” where children with eczema or dermatitis may later be more likely to develop allergies. It is also part of the bigger argument that healthy barriers matter everywhere in the body, including the skin and gut.
That is why the conversation repeatedly links skin microbiome health with:
- Gut integrity
- Immune regulation
- Inflammatory load
- Hormone balance
- Long-term resilience
Rethinking Moisturizers and Supportive Skincare
One of the more practical parts of the episode is the discussion about moisturizers. Kiran argues that many lotions are water-based emulsions that may temporarily reduce moisture loss but do not necessarily repair the deeper barrier issue. He emphasizes the importance of the ceramide layer and suggests that lipids may be more useful than many standard water-heavy formulations.
The episode also discusses potential support from:
- Simpler moisturizers with fewer ingredients
- Skin-mimetic lipids
- Avoiding unnecessary fragrances
- Avoiding overly harsh preservatives and antimicrobial-heavy formulas
- Supporting the body internally with dietary fats and phyto-ceramides
There is also a strong theme of reducing overwhelm. Rather than throwing everything away, listeners are encouraged to start with one product and choose cleaner, simpler options where possible.
The Case for Less, Not More
If there is one practical philosophy that stands out in this conversation, it is this: more skincare is not always better skincare.
That applies to:
- Multistep routines
- Excessive washing
- Over-exfoliation
- Fragrance-heavy products
- Repeated barrier disruption
- Constantly trying to “fix” the skin with aggressive inputs
Instead, the episode encourages a more restrained approach that respects the skin’s natural biology. That message may resonate with listeners who feel burned out by trends, conflicted by skincare marketing, or frustrated by routines that promise glow but leave the skin increasingly reactive.
This Episode Is Brought to You By
Dr. Brighten Essentials Myo-Inositol Plus— a research-backed formula designed to support hormone balance, metabolic health, and ovarian function. Featuring the clinically studied 40:1 ratio of myo-inositol to D-chiro-inositol, it helps promote healthy ovulation, improve insulin sensitivity, and support more regular cycles—making it a powerful daily tool for PCOS, fertility, and overall hormone support.
Exclusive for podcast listeners: use the code POD15 for 15% off your order. Shop now
OneSkin
Founded by an all-woman team of PhD-level scientists, OneSkin is revolutionizing aging with the OS-01™ peptide, the first ingredient proven to reverse skin’s biological age by targeting cellular senescence. The result? Skin that looks, feels, and acts younger. It’s never too early — or too late — to invest in your skin health.
Use code BRIGHTEN for 15% off your first purchase. Shop now
Links Mentioned in This Episode
- Kiran Krishnan’s Instagram: @kiranbiome
Related Articles
- Comprehensive Guide to PCOS Skincare: Expert Strategies for Radiant, Clear Skin
- What Causes Rosacea on Face: Treating Rosacea Naturally
- Estrogen Face Cream: A Hormone-Boosting Treatment for Healthier Skin
- Acne in Pregnancy: What to Do When You’re Pregnant with Acne
- Autoimmune Progesterone Dermatitis (APD): Symptoms, Causes, Foods to Avoid, and Treatment Options
- Acne and Polycystic Ovary Syndrome: Hormone and Skin Care Treatment
- Acne After Stopping Birth Control & How To Treat It
- The 10 Best Vitamins and Supplements for Hormonal Acne
- Want to Treat Hormonal Acne Naturally? Things to Try Before Birth Control
Related Episodes:
- OneSkin Founder Carolina Reis Oliveira: Peptides for Hair Loss & Skin Aging Reversal
- Dr. Sara Cherem: The Best Skincare for Aging Skin: Dermatologist Secrets You Haven’t Heard Before
- Dr. Tony Youn: Unlock the Best Skincare Products for Aging Skin + Tips to Reverse Collagen Loss Naturally
- Jen Fugo: Natural Treatments for Eczema That Actually Work: Creams, Moisturisers & More
- Dr. Brighten: Estrogen Cream for the Face: What the Science Says About Anti-Aging, Collagen, and Hormones
Research and Study References Mentioned in the Conversation
Furman D, Auwerx J, Bulteau AL, Church G, Couturaud V, Crabbe L, Davies KJA, Decottignies A, Gladyshev VN, Kennedy BK, Neretti N, Nizard C, Pays K, Robinton D, Sebastiano V, Watson REB, Wang MC, Woltjen K. Skin health and biological aging. Nat Aging. 2025 Jul;5(7):1195-1206. doi: 10.1038/s43587-025-00901-6. Epub 2025 Jun 17. PMID: 40527938.
Kim RW, An Y, Zukley L, Ferrucci L, Mauro T, Yaffe K, Resnick SM, Abuabara K. Skin Barrier Function and Cognition among Older Adults. J Invest Dermatol. 2023 Jun;143(6):1085-1087. doi: 10.1016/j.jid.2022.11.023. Epub 2023 Jan 11. PMID: 36641132; PMCID: PMC11739001.
FAQ: Skin Aging Treatment and Skin Microbiome
The skin microbiome refers to the community of microorganisms that live on the skin. In this episode, it is described as an important part of maintaining pH, supporting barrier function, and helping the skin stay balanced.
In the context of this episode, “leaky skin” refers to skin barrier dysfunction or increased permeability. The idea is that when the barrier is compromised, moisture escapes more easily and irritants or inflammatory triggers may penetrate more deeply.
According to the discussion, possible signs include dryness, flakiness, thin-feeling skin, hyperpigmentation, early fine lines, and difficulty keeping skin hydrated.
This episode suggests that supporting the skin microbiome may help maintain pH, reduce unnecessary disruption, and support healthier barrier function. That may matter not only for appearance, but also for long-term skin resilience.
The conversation highlights that hormones influence skin hydration, inflammation, acne, and visible aging. Hormonal shifts may make barrier dysfunction more likely or more noticeable.
Yes. A major theme of the episode is the gut-skin connection. Kiran discusses how gut barrier health, inflammation, immune responses, and microbial activity may all influence what happens in the skin.
Not according to the core message of this discussion. The episode repeatedly challenges product-heavy routines and suggests that for many people, a simpler approach may better support the barrier and skin microbiome.
Based on the episode, a reasonable place to start is simplifying personal care products, reducing unnecessary irritation, and choosing gentler, cleaner skincare options.
Transcript
Kiran Krishan: [00:00:00] Barrier dysfunction in the skin is an independent risk factor for Alzheimer's and dementia. They're showing that it's more associated with barrier dysfunction on the face rather than say the arms and the legs and probably the part of the skin, especially women irritate the most because of all the things that they do.
Dr. Brighten: Wanna talk about that Baltimore study and what we learned about skin aging and inflammation in the body.
Kiran Krishan: What was fascinating about it is they found that age skin was one of the best predictors for mortality and morbidity in individuals.
Narrator: Karen Krishnan
Narrator 2: is one of the most influential voices in microbiome science.
Known for translating cutting edge research into real world results.
Narrator: A research
Kiran Krishan: microbiologist and leader in microbiome therapeutics.
Narrator: He's uncovering the hidden link between gut health and leaky skin
Dr. Brighten: and why it may be the missing piece in anti-aging. How do I know if I have leaky skin? What are the signs and symptoms they could look for
Kiran Krishan: if you're seeing a lot of hyperpigmentation on your skin?
The [00:01:00] hyperpigmentation is a example of senescent. Senescence is where cells become zombie cells, essentially.
Dr. Brighten: Aged skin is increasing your risk of death. What is the worst thing women are doing to their skin on a daily basis?
Kiran Krishan: All the ing of the skin is probably causing more harm than good. Mm-hmm.
Dr. Brighten: What is the biggest lie women are told about skincare?
Kiran Krishan: Well, I think one of the biggest things is that your skin is gonna age, right?
Dr. Brighten: Wait, are you saying it's never gonna age?
Kiran Krishan: Well, it can, you can dramatically slow down the aging.
Dr. Brighten: Okay. Okay. Because I was like, I'm all in. If you say never,
Kiran Krishan: I wish never, but, but the thing is that. That the, the formation of fine lines, wrinkles, dryness, hyperpigmentation, and all that is inevitable.
Mm-hmm. Right. They're associated with an aging process and that the way to overcome them is by masking them with more things. Right. So fillers and, you know, [00:02:00] Botox and all of that. Mm-hmm. That, that's the only way you can do it or covering it up. Right. And so. To me, there's, there's this, uh, hopefully we can lead a little bit of a mind shift where making skin look better by making it healthier.
Dr. Brighten: Mm-hmm.
Kiran Krishan: Rather than simply the act of trying to make it better looking. Right. Um, and so because we can make skin look good, there's many different tactics to it, make up and surgery and all of that. But are we actually making it healthier? Mm-hmm. And the, and the funny thing is we don't do that with any other hor uh, with any other organs in our system, right?
Yeah. We don't mask dysfunction in the ho, in the, in the organs, um, just to try to make the organ look better. But the skin is an organ and we forget that, and we forget its role as a barrier. And so we kind of skip over all of those important features of it. Um, and then we just want to make it better like a veneer, if you will.
And so I think, I think one of the misconceptions and one of the lies is that you cannot [00:03:00] improve your skin without. All of those procedures and tactics and so on. Mm-hmm. You know, I think you can, I think there's more natural ways that you can do that.
Dr. Brighten: Okay. We're gonna get into those today. Yeah. But we wanna talk about that Baltimore study and what we learned about skin aging and inflammation in the body.
Kiran Krishan: What was fascinating about it is they found that. Aged skin was one of the best predictors for mortality and morbidity in individuals. Mm-hmm. Right now in our world, we would normally, and if you said this to me eight years ago, nine years ago, I'd go, well that makes sense because the skin is a reflection of the inside, right?
Yeah. So their skin is aged because they're unhealthy on the inside. Sure. Yes. They're gonna be more sick.
Dr. Brighten: Mm-hmm.
Kiran Krishan: They found that no, that's not actually true. In fact, the age skin precedes any biomarkers that they could find on the inside that would lead to any disease pathology. And so the skin dysfunction started first.
Dr. Brighten: Mm-hmm.
Kiran Krishan: Now they were able to correlate also then skin dysfunction with very specific conditions like bone health. Right. [00:04:00] Like who would've thought your skin has an impact on bone health?
Dr. Brighten: Well, I mean, we generate vitamin D there. So that shouldn't have been a total leap. Right? But it is much deeper than that.
It's, I, I know my listeners are savvy and gonna be like, oh, vitamin D, but it actually goes way beyond that. It goes way
Kiran Krishan: beyond
Dr. Brighten: that about the actual function and barrier of the skin being compromised.
Kiran Krishan: Yeah, it's a barrier of the skin being compromised, thereby allowing in pro-inflammatory, you know, antigens and mediators and toxins and all that to actually get into the skin.
Past the stratum corneum, which is a very top, closer to the dermal layer. Mm-hmm. So, um, if, if the audience isn't familiar, you've got the stratum corneum, the very top, you've got the epidermal layer and then the dermal layer. Right? So the skin has these multiple layers. The immune system functions in both the epidermal and the dermal layer.
And so if things penetrate far enough into the layer of the skin, it's gonna elicit an immune response. 'cause the skin acting as a barrier shouldn't see those antigens in there.
Dr. Brighten: Mm-hmm.
Kiran Krishan: And so. When things penetrate far enough, [00:05:00] they can elicit enough of an immune response starting in the skin that actually then spreads throughout the rest of the body.
And in fact, like for example, psoriasis, this is a, it's a perfect example, right? In a psoriatic, a psoriatic lesion, there are immune responses that are occurring, right? So, so the immune system's attacking their own, your own parts of your skin. There are these proteins that are being generated in these psoriatic lesions that are very specific to a psoriatic lesion.
You find those same proteins in bone where there's inflammation that's starting the process of osteoporosis. Mm-hmm. Right. So there's a real connection here between inflammation starting at the surface and then penetrating throughout the rest of the body. And perhaps proteins and other components of the inflammation from the skin traveling throughout the body and eliciting more inflammatory responses elsewhere.
Dr. Brighten: Mm-hmm.
Kiran Krishan: Right. So then what the study concluded was age skin was an independent risk factor [00:06:00] for morbidity and mortality, looking at age-related chronic conditions, right, independent. Us outside of obesity and everything else, right? It's on its own. It's an independent risk factor.
Dr. Brighten: So if aged skin is increasing your risk of death, what is the worst thing women are doing to their skin on a daily basis?
Kiran Krishan: So if you think about all the sterilizing of the skin, right? So we wash our skin with all of these antimicrobial soaps and, you know, uh, benzo, peroxides and all that. So we're, we're, we're. Pulling off the layer of microbes, protective microbes of our skin. Mm-hmm. Thereby, and then also, um, you know, removing the top layer because a lot of people do, you know, uh, exfoliation and all of these things, right?
So we're like peeling off the top layers of the skin and then putting on toxigenic compounds on top of it. Right? Mm-hmm. That have all kinds of benzo, like, uh, um, you know, they have plastics, microplastics in it, uh, pesticides, herbicides, you know, all of these chemicals [00:07:00] that you find, um, that are found within personal care products that all can be toxigenic damaging to the skin, drying out the skin.
And we also don't know what. Things like microneedling and all actually do to the skin eventually. Right? Because we're penetrating those barrier systems. And I had a great conversation with a plastic surgeon that is starting to become more skin microbiome conscious.
Dr. Brighten: Yeah.
Kiran Krishan: And she was starting to get really nervous about all of the microneedling and injections and all that they do, because it's really unusual to do that much damage.
Right. It's completely unnatural. Mm-hmm. To be doing that much damage, that depth. Of the skin, maybe a little bit of, uh, microneedling at like 0.25 millimeters or something like that. Yeah. That'd be just okay. Right. We, we have hair loss studies and all that on that, but the depth that they're going into, I think is probably causing more harm than good.
Mm-hmm. Because you're breaking that barrier quite significantly.
Dr. Brighten: Well, you're breaking that barrier significantly and then. It's also, no one talks about the other [00:08:00] products being used around it when the barrier gets compromised in that way. Mm-hmm.
Kiran Krishan: Right. We can, we can hypothesize that they likely damage it.
Dr. Brighten: What I wanna ask you is that you're really trying to shift the paradigm away from, you just have damaged or aging skin and talking more about the phenomenon of leaky skin. Yes. Can you tell us more about that?
Kiran Krishan: We mentioned skin is a barrier. That's, it's one of its primary roles. Um, it's in fact one of the largest barriers in your body you come to realize is that any part of the body that's a barrier that starts to become dysfunctional.
Meaning it starts becoming more permeable than it should leads to complications and disease. There's been this really well thought. Through and proven concept called the atopic march, right? So this is kids with eczema and psoriasis. E, especially eczema or some form of dermatitis, tend to have a barrier dysfunction in their skin.
As a result of that food and environmental antigens actually leak through the skin and the immune [00:09:00] system meets those antigens in the periphery. As a result of that, you lose all of the ability of developing oral tolerance to them. Mm-hmm. So they develop hypersensitivity to all of these antigens. Right.
So a kid who has dermatitis, who's born with dermatitis, has a eightfold higher risk of developing severe allergies, uh, against food particles, environmental particles, and so on. That's called the atopic march, and and dermatologists have known about it for some time. There's a few groups that are working on solutions for the atopic march.
We've known that the skin as a barrier can become compromised. Things can actually leak through. Mm-hmm. And when they leak through, they're entering into our system in a place where they shouldn't be. And the immune system does not like that. And it freaks out. Right. So anytime the skin barrier becomes compromised, I think we start to see a number of issues that mm-hmm.
That develop.
Dr. Brighten: Well, what's interesting is that. As we've begun to understand this connection of actually developing allergies via the skin barrier. Mm-hmm. We've seen the [00:10:00] shift in pediatricians recommending that we delay food. Right? Yeah. So if you can define oral tolerance that you had mentioned earlier.
Kiran Krishan: So oral tolerance is a beautiful, magical system where, um, when you. Sample, say food. Let's take a peanut, a antigen, right? Um, when you sample it through your digestive tract, there are mechanisms involved in your digestive li tract lining that allows your immune system to sample these antigens and then get cues from the microbiome that this is fine.
And then it upregulates a type of part, a part of your immune system called a treg system. That treg system suppresses any unwanted immune responses against it, right? So the, to get more technical about it. You've got this antigen that comes in the microbiome if you have a healthy microbiome, is producing things like short chain fatty acids, inducing more iga, a immunoglobulin A, which can bind to these antigens and kind of neutralize them and kind of mask 'em as, Hey, this is not a problem, right?
Mm-hmm. Then you've got these immune cells called dendritic [00:11:00] cells that reach across the lining of the gut. They sample all these things that are in the mucus layer. When they sample something in the context of short chain fatty acids and iga a they, they upregulate a type of T cell called a treg cell.
That treg cell builds memory and tells the rest of the immune system don't attack this thing. That's called oral tolerance. Right. So this is how we're supposed to encounter most antigens, certainly food-based antigens.
Dr. Brighten: Mm-hmm.
Kiran Krishan: Because the skin is supposed to be a barrier antigen, cis land and brush off of it.
Right. But we inhale things every day. We things go through our eyes, and that's why our eyes, our nose, our ears, all draining to the back of our throat, right? And we swallow all of those components and so we sample it through the gut. That is sampling for oral tolerance. We don't have those same treg cells.
We don't have those same dendritic cells. In our periphery. So when we, when a, when a food-based antigen enters through the skin and enters in the peripheral area, it activates an innate [00:12:00] immune response. Like natural killer cells, basophils, oph, fills all of these like really freaking out panicked immune cells, right?
Mm-hmm. That, that are seeing something that shouldn't see in a location that it shouldn't be in. And so they elicit a hypersensitivity. Very inflammatory response to it. And so you lose that learning from the treg cells. Mm-hmm. Now, this process is so important that the Nobel Prize in 2025 for physiology and medicine was given to three scientists that discovered this whole oral tolerance, treg mechanism.
You know, and so when they're doing those studies and they're trying to look at. If we put an antigen on the skin of an animal, can we see antibody responses inside the animal against those antigens, right? Mm-hmm. That's what they were trying to figure out.
Dr. Brighten: Yeah. And for people listening, this is when medicine realized that all of the recommendations of delay, peanuts, delay, you know, eggs.
Mm-hmm. All of that was actually creating. Food allergies and children rather [00:13:00] than actually preventing 'em. So, I mean, Nobel Prize, of course. Yes. It's like a really big phenomenon because generations were impacted by that. Yeah. And that's why I think it's so important in the context of this conversation, what I wanna ask you, if people listening right now and they're wondering.
How do I know if I have leaky skin? How do I know if I have barrier dysfunction on my skin? Yeah. What are the signs and symptoms they could look for?
Kiran Krishan: So you, you wash your skin, let's say with, with regular soap. And, and let's say you don't put lotion on it. Um, if your natural skin tends to be quite dry and what we call.
Thin skin. Mm-hmm. If you have, if you're developing a lot of fine lines and wrinkles prior to the age you think you should be.
Dr. Brighten: Yeah.
Kiran Krishan: Um, so if you're in your late twenties, early thirties and already developing fine lines and wrinkles, if you're seeing a lot of hyperpigmentation on your skin, uh, the hyperpigmentation is a example of senescence.
Mm-hmm. That's on your skin, right? Mm-hmm. Senescence is where cells become zombie cells essentially. So your, your melanocytes that are producing the melanin are. Undergoing a lot of, of oxidative [00:14:00] stress and damage. And as a result of that, they're kind of becoming dysfunctional and becoming zombie cells and just sitting there and producing melanin.
Mm-hmm. And so that's a sign that there is a significant amount of damage occurring in the skin. Um, they used to call those age spots Right. For a reason as, because usually with age comes these dysfunctions, but now you're seeing it in younger and younger individuals. Mm-hmm. So the condition of your skin will tell you whether or not it's leaky.
The, the most common one is, is dryness and flakiness in the skin.
Dr. Brighten: Mm-hmm.
Kiran Krishan: Right. So if your skin is, is, uh, now, if it's been like that all your life, there's some people that just have really low oil production and a poor ceramide layer. Right. So their, they've, their skin has been dry their entire life.
Mm-hmm.
Kiran Krishan: That's a little bit different than, let's say you're in your twenties, thirties, forties, and you're noticing that your skin is getting drier and drier and it's harder to keep moisture on your skin. Of course, we're using topical lotions and things that kind of mask it. They don't really moisturize the skin in the way we think they do.
Um. But if you, if [00:15:00] you're, if you're doing all of those things just to maintain some degree of moisture in your skin and you're losing, uh, you're losing moisture very fast, it's likely becoming, um, leaky. One of the ways in which we test for leaky skin is something called twi, TEWL, trans Epidermal Water Loss.
It's a device that actually measures how much water your, your skin loses. Mm-hmm. And that is a really strong surrogate marker for skin barrier. Function. Right. So looking at the dryness is really important.
Dr. Brighten: Yeah. If topical lotions are not hydrating our skin, what actually does?
Kiran Krishan: Yeah. So that's a, that's a great question.
Right. So I'm, I'm actually in the process of trying to develop a, uh, a moisturizer that you're like, actually, you're gonna make it, I'm gonna make that thing right. But here's why, because most topical lotions are water-based. Systems, they're emulsions, right? Mm-hmm. And the way the skin is designed is things aren't supposed to penetrate through from the up, from the outside in, nor is moisture supposed to penetrate out from the inside out.
[00:16:00] What, how do we prevent moisture from penetrating out? Well, we have this fatty acid mortar layer called the ceramide layer, right? The ceramide layer binds all the cells, the skin cells together. So you've got this, um, hydrophobic layer that's acting as a barrier that prevents. Evaporative, uh, moisturize, losing moisture through evaporation.
Mm-hmm. So then the moisture can't come outta the skin. Now, if your skin is getting dry really easy, it means that ceramide layer is broken, right? Mm-hmm. And it's getting dry because evaporation is, is drying out your skin easily. So when you put lotion on, which is a water-based system, most of the time with an emulsion in it, you're, you're actually not getting any sort of.
Barrier fix because the lotion is temporarily preventing that water loss. Mm-hmm. That's why your skin feels a little more moisturized, right? Because it's acting as a cap to preventing the moisture loss. But then once the moisture in the lotion evaporates, it goes back to feeling dry again. Right. And so, one of the best things you can do, actually, so if you, if you're able to [00:17:00] use lipids on the skin.
That's much better. Mm-hmm. Right. Lipids will penetrate a little bit further in and will help hold moisture in better. So we're, we're trying to work on and develop an anhydrous, uh, lotion. Mm-hmm. Which means a lotion with no water in it, but it also can't be a thick enough liquid that occludes your pores and creates comedones, which just creates commodos, which just creates lesions and all that.
So it has to be thin skin, mimetic, lipid. Mm-hmm. Right. There's not anything out there right now, so people just have to use the lotions that they have and maybe use some oils or things like that from time to time. The other thing you can do is actually improve your liver health.
Dr. Brighten: Mm-hmm.
Kiran Krishan: And take in enough, um, uh, phyto.
Ceramides, right? So, so certain, uh, fibers, so bran, rice, bran, and other fibers. So rye and things like that. Have these compounds in it called phyto, phyto ceramides that your liver will convert to the type of ceramides that you have in your skin and it'll [00:18:00] transport it to the skin to replace the ceramides that you're missing, right?
So most people wouldn't, wouldn't connect their liver health with their skin health, but it plays a really important role, right? Mm-hmm. So if you're naturally really dry. Make sure your liver is healthy. Take your turmeric, your milk thistles, your dandelion roots and all that to make sure your liver is healthy and get enough of the phyto ceramides into your diet.
Dr. Brighten: You just mentioned gluten containing products. Yeah. Are there ways to get those phyto ceramides that are not gluten containing foods?
Kiran Krishan: Yeah, you can get it from rice. As well. Okay. Yeah. Rice, brown Rice. Brown rice. Yeah. Brown rice. Mm-hmm. Has phyto ceramides in it as well. Perfect. Um, and if you're not gluten intolerant, you can have it from time to time and, and get the ceramides in there.
Mm-hmm. But the liver plays such an important role in that, right? So the liver can also take, um, fatty acids from the diet and produce ceramides out of it. And so if you're getting, as long as your liver is healthy, you'll still start producing enough ceramides. To replace the skin, what you're losing on the skin.
Dr. Brighten: And when you say fatty acids, what kind are you talking about specifically?
Kiran Krishan: So, so [00:19:00] normally like, um, lipids from things like, um, olive oil and so on, this is one of the reasons why olive oil tends to be really good for the skin.
Dr. Brighten: Mm-hmm.
Kiran Krishan: Um, so, so having your, a good measure of omega threes. Omega six,
Dr. Brighten: yeah.
Kiran Krishan: They can be actually metabolized. And reconstructed into ceramides.
Dr. Brighten: Yeah.
Kiran Krishan: For the skin,
Dr. Brighten: which for people listening, Omega-3 fatty acids, it's also been found people have higher Omega-3 content when they're measured in their blood, have lower levels of IGF one contributing to acne. Yeah. And so you see that correlation.
So you get a two for one, you
Kiran Krishan: get to one the, the inflammation goes down. Mm-hmm. And so on as well. Yeah.
Dr. Brighten: Let me ask you, why do women tend to have more skin barrier dysfunction than men? Yeah.
Kiran Krishan: Well, I think in part because women actually treat their skin a lot more with a lot more things.
Dr. Brighten: How many? It's like 13 products a day.
Right?
Kiran Krishan: Exactly.
Dr. Brighten: Is there anything more to it, or is it just like how much we have been influenced. To treat our skin.
Kiran Krishan: I think hormones play a big role as well. Right? So, um, hormones have a, have, have a, a dramatic effect on the skin as they do with [00:20:00] everything else in the body. So women have that unfortunate side of having, uh, more complications with hormone imbalance than men do.
Dr. Brighten: Yeah. Okay. We're gonna talk hormones every once, so just hang tight. But I wanna ask you, what about these influencer, like 13 step night routines or wearing masks? Yeah, overnight, like the some things they're hyaluronic, sometimes they're like Korean glass skin. I don't even know what's in that, but what are your thoughts about what that's doing to the skin barrier and also the microbiome?
Kiran Krishan: Yeah. I think it's so unnatural to have that on your skin for that long a period of time, right? Mm-hmm. I don't think people need to sterilize their skin. Now, if you're dealing with really bad cystic acne or something and you're on a procedure, or you're on a protocol for cleaning your skin, benzo peroxide or whatever it may be, that's a different thing, but.
But normal day-to-day routines, I don't think you need to sterilize your skin. Mm-hmm. Right. So maybe a light soap, maybe to get some of the dirt off. Um, and then hopefully, uh, a skin mimetic, uh, moisturizer and, uh,
Dr. Brighten: what a skin mimetic for people listening.
Kiran Krishan: [00:21:00] So, skin mimetic means it mimics the, uh, the type of oils that are produced on the skin.
So they're normally. Very thin, high penetrating oils. Right? So like glycerol, capite is a good one, or caprylic acid is another good one. Mm-hmm. Um, so if you find like a moisturizer that is based on gris, glycerol capite or caprylic acid, they tend to be much more skin mimetic. Mm-hmm. Uh, they're thin, they don't occlude, they don't create comedones, which are the A lesions.
Um, and, and they're just really healthy for your skin in that, in that format. Um, so light moisturizer, light cleaning. Sleep.
Dr. Brighten: Mm-hmm.
Kiran Krishan: Right. And that's it. Um,
Dr. Brighten: and then how about in the morning?
Kiran Krishan: Same thing I would say.
Dr. Brighten: Okay.
Kiran Krishan: Yeah,
Dr. Brighten: because I have seen, I gotta say there's, uh, like the Korean skincare routine, the Japanese, these Asian women are like, you wake up in the morning and it's just cold water on your face.
Kiran Krishan: I would say. Nine outta 10 times. I don't actually wash my face in the morning. Mm-hmm. It's, it's cold water and just regular water,
Dr. Brighten: so seriously. Right. Every time I have a skin expert on, or like a [00:22:00] dermatologist, they will talk about how they don't wash so much.
Kiran Krishan: Yeah. Everything where we've hyper sterilized.
Components of our body, our home, everything. Right? Where we've warded off microbes, we start to see dysfunction occurring. Mm-hmm. Because what we forget is microbes play such an important role in every aspect of our health, including our skin. Right. There's so many functions. On our skin that we cannot do ourselves.
For example, I'll just give a quick example of that. It's really important to maintain a very narrow pH range on your skin.
Dr. Brighten: Mm-hmm.
Kiran Krishan: Right? You want your skin to be slightly acidic. It's around four to 4.5 ish. It can be a little bit lower than that, but the main reason you don't want it to be more neutral or even basic is because you'll get fungal overgrowth on your skin all the time.
Mm-hmm. Right? There are mold spores and all that all over the place. They settle on our skin That will easily grow. If our pH was any higher, the way we maintain pH on our skin is we have beneficial microbes on our skin that break down the oils into [00:23:00] from, uh, and take out the fatty acids, and they make fatty acids from the oils that are being secreted and those fatty acids.
Lower the pH of the skin.
Dr. Brighten: Mm-hmm.
Kiran Krishan: Right. So something so foundational to the, to the structure and function and look and barrier function of our skin. Microbes do that for us if we knock those microbes down consistently and their numbers are not, um, where they should be. We lose pH balance on our skin.
Mm-hmm. Then you see all these products about pH balance, pH balance, and you need to use products to
Dr. Brighten: balance
Kiran Krishan: Yeah. Your pH on the skin. Right. So it's just a, a, an elegant example of how nature, just in this symbio way, we've got this beautiful relationship with these re resident microbes on the skin, maintain the healthy terrain.
Dr. Brighten: Mm-hmm.
Kiran Krishan: By controlling the pH. Same thing in the gut. Okay.
Dr. Brighten: Let's talk about the role hormones are playing mm-hmm. In skin barrier dysfunction.
Kiran Krishan: Yeah. So, I mean, we, I think most people understand that hormones have an impact on the skin, right? So we see [00:24:00] hormonal acne, for example. Mm-hmm. Um, you know, we, we see topical.
Skin topical hormone use, which is awesome, right? Because, and, and we know that that estrogen has a very positive impact on the skin. We, we talked about, we mentioned the pregnancy glow earlier on, um, you know, before we got on, and, and, and that's a hormone related function of the skin where mm-hmm. You're looking, you have a glow to your skin, you moisturize skin, looks, plumper, fewer, uh, fine lines and wrinkles.
So we know that an improvement or balanced hormones has a very positive effect on the skin. An imbalance hormone profile has a detrimental effect of the skin. Mm-hmm. Can be very inflammatory, can dry drive dryness, fine lines, wrinkles, which is another. Indication of AIDS skin. Right. And, um, significantly AIDS skin, especially before the time you would expect is, uh, is correlated with Dr.
Drastic hormone dysfunctions.
Dr. Brighten: Mm-hmm.
Kiran Krishan: Right? So when [00:25:00] you looked at conditions like PCOS and all that, that are very inflammatory, those conditions have a direct inflammatory impact on the skin as well.
Dr. Brighten: So lemme ask you, 'cause with PCOS, there is a large portion of women who will develop cystic acne. Yeah.
They have inflamed skin. There is going to be skin barrier dysfunction. Yeah. How like, I have yet to see a study. I don't think it exists. If PCOS is leaving to skin dysfunction Yep. Is the skin dysfunction may be contributing further to the inflammation that's associated with PCOS.
Kiran Krishan: I think that's a great connection.
Right. Because I think that's a, that's a cyclical effect.
Dr. Brighten: Mm-hmm.
Kiran Krishan: Um, and, and. PCOS is pro-inflammatory profile leading to cystic acne and other, you know, um, lesion generating issues, right? All of that is directly related to how inflammation from the gut and PCOS has a big metabolic component, a big gut component to it, right?
Mm-hmm. Inflammation from the gut has, has been shown to directly impact [00:26:00] in, uh, sebaceous glands, increasing the amount of. A CBU that's produced and increasing the inflammatory response in the pore itself. Mm-hmm. Right. Um, and you actually see LPS, 'cause I would guess, uh, that the vast majority of women, PCOS probably have leaky gut and thereby endotoxins LPS leaking through are actually.
Found in sebaceous glands in the skin.
Dr. Brighten: Mm-hmm.
Kiran Krishan: Upregulating an inflammatory response in addition to the increase in sebum that's being produced. Right. So that, that double whammy where you're getting both inflammation and extra sebum is creating a clogg pour with an inflammatory response. Right. So you get these inflammatory lesions, not non-inflammatory lesions.
Mm-hmm. When we did, um, we did a. Two acne studies before I, I left Microbiome Labs. Um, and our whole hypothesis was that. If we fix the lining of the gut and we stopped LPS translocation and [00:27:00] we increased acetate production, which is one of the short chain fatty acids
Dr. Brighten: mm-hmm.
Kiran Krishan: That we could bring down acne, inflammatory and non-inflammatory lesions.
Right. Uh, and we showed in, in two studies, including a second one, which is a 90. Study a 75% reduction in non infl, in inflammatory and non-inflammatory lesions just by using a probiotic in the gut.
Dr. Brighten: Okay. So you did nothing else but a probiotic in the
gut.
Kiran Krishan: Gut did nothing else. Yeah. Yeah. We, we did, uh, the, the, the MegaSpore or a version of the MegaSpore that I adjusted, um, to, to do two things.
Number one, to increase the production of short chain fatty acids and specifically increase acetate mm-hmm. Rather than butyrate, because what we found is that. There was evidence that, uh, acetate becomes, goes out into circulation way more than butyrate. Most of butyrate is used in the gut.
Dr. Brighten: Mm-hmm.
Kiran Krishan: Acetate can be found actually in skin, reducing inflammation in the, in the sebaceous glands.
And acetate can also act as an antimicrobial mm-hmm. To kill [00:28:00] down some overgrowth in the pores. So we said, okay, we can stop LPS and we can increase acetate. We're surely gonna see a dramatic improvement in the skin. And we saw 75% reduction in lesions, which is on par with any antibiotic study on acne.
Mm-hmm. So that was really exciting to see. So that gave like a really clear gut skin connection.
Dr. Brighten: Yeah.
Kiran Krishan: But it also spoke to why certain hormone conditions would probably create so much problem on the skin is because they're, they're also associated with dysfunction in the gut. Systemic inflammation and so on.
Dr. Brighten: Are there certain foods people could consume to improve, improve their acetate production?
Kiran Krishan: Yeah, so, um, fiber and prebiotics in general will increase acetate production, um, but pectin. Pectin, which is a fiber from fruits mm-hmm. Seems to increase, um, acetate production on its own. This may be why some juices maybe have been associated with improved skin.
Dr. Brighten: Mm-hmm.
Kiran Krishan: Pectin specifically from [00:29:00] fruits does increase acetate production,
Dr. Brighten: and every woman with PCOS is told not to eat fruit by. Well-meaning doctors. Mm-hmm. Sometimes, and well-meaning influencers, but they're told like, if you wanna control your blood sugar, never eat fruit. Yeah. Uh, it's, it's, um, a bit backwards sometimes.
It's how we approach things. Right.
Kiran Krishan: Yep.
Dr. Brighten: I wanna ask you, we're seeing it talked about more now, and that's using. Estrogen topically on your face. What are your thoughts in terms of the barrier protection? The microbiome?
Kiran Krishan: Yeah. You know, estrogen is like, the more you learn about, it's such a miracle thing, right?
You think about all the protection it affords women prior to starting a decline in estrogen production, right? So when, when women start to see a decline in estrogen production, in perimenopause, you start to see gut barrier function going off. You start to see, um, increased risk for osteoporosis, cardiovascular disease, all of these things that men were suffering from a little, uh, earlier.
Mm-hmm. Women are starting to catch up to men at that point, and it's all with [00:30:00] estrogen declining. So it's, it's so surprising to me every time we find out. Another cell, another tissue that has an estrogen receptor Yeah. On it. So I think topical estrogen is an amazing thing. Mm-hmm. That women should be absolutely utilizing.
Right. But with so many things with hormones have been misdirected and misinformed for so long about it.
Dr. Brighten: Yeah. I wanna talk about what do we know about skin barrier dysfunction and cognitive decline, especially in women, the
Kiran Krishan: Baltimore Longitudinal Study, there's. Data that has come out that, that shows that barrier dysfunction in the skin is an independent risk factor.
Right. For Alzheimer's and dementia. Mm-hmm. And, and like neurodegenerative conditions in general. Um, in part it's because, and, and, and they're showing that it's, that it's more associated with barrier dysfunction on the face. Mm-hmm. Right. Rather than say the arms and the legs,
Dr. Brighten: which is what is most exposed at all
Kiran Krishan: Exactly.
Dr. Brighten: All times, right? Yeah.
Kiran Krishan: And probably the part of the skin that, that especially women irritate the most. Mm-hmm. Because of all the things that [00:31:00] they do. Right. So if you think about that part of the skin getting the most amount of sterilization, the most amount of compounds and chemicals and all of that stuff, and most amount of procedures that are being done to it.
As that part becomes, as the, the face and neck becomes more and more, uh, dysfunctional in terms of a barrier, you start to get, uh, compounds that leak through that actually are associated with triggering inflammatory processes in the central nervous system.
Dr. Brighten: Mm-hmm.
Kiran Krishan: Right. Which is really mind boggling when you think about it.
Dr. Brighten: Yeah.
Kiran Krishan: Um, and scary. You would, you would not necessarily connect that.
Dr. Brighten: Totally. I told you my trip to PubMed was not a good time.
Kiran Krishan: No. And fungal overgrowth is another risk. Mm-hmm. Right. So malthe is another issue when they, when that overgrows in the skin, which is another skin pH balance issue. Mm-hmm. Um, you know, when you start, uh, losing the barrier function, the skin dries out too much.
All of that stuff can leak through and it's right there in the central nervous system when it, when things enter your sinus cavities and all that. Yeah. It can make [00:32:00] its way to the brain quite easily and trigger these inflammatory responses that can lead to the type of neurodegenerative. Process that we're used, we're used to seeing, you know, and so, so it's, it's bog mind boggling to me that skin dysfunction is associated with it, but it's a great predictor.
Dr. Brighten: Mm-hmm.
Kiran Krishan: Of the risk of developing neurodegenerative conditions.
Dr. Brighten: I'm curious, has there been any link to Parkinson's disease? Have you seen any research with regards to Parkinson's?
Kiran Krishan: No, but I would, I would be surprised if it's as related to Parkinson's as it is to Alzheimer's, right? Mm-hmm. Um, and part of that reason is because.
Parkinson's typically starts in the enteric nervous system. Mm-hmm. In the, which is the neurological system that covers the full digestive tract. It's always often thought of as a second brain. So there's a, just like in the, uh, in the brain, they look at amyloid beta plaques. Right. They look at this misfolding of proteins as one of the signals that, okay, there's enough dysfunction occurring.
We're, we're, uh, losing something called proteostasis. So the, the cells in the brain aren't dividing properly, [00:33:00] they're degenerating too fast, and they can't. Replicate themselves, right? So you can't regenerate the tissue. So they're, they've been using that protein as a marker for it. In Parkinson's is a different type of misfolded protein called alpha-synuclein, but they always measure it first in the enteric nervous system.
Mm-hmm. So for Parkinson's, it starts in the gut and, and that's why it's pretty well established now that one of the first signs of Parkinson's is chronic constipation.
Dr. Brighten: Mm-hmm.
Kiran Krishan: Right. And then they can actually measure that alpha-synuclein moving up the vagus nerve. The next place where it becomes really apparent is when it hits the olfactory nerve and you start losing the sense of smell.
Dr. Brighten: Mm-hmm.
Kiran Krishan: Right. So, so, um, I remember, uh, Tom O'Brien had this like flip book of smells. I don't know if he ever showed you that. No.
Dr. Brighten: But it doesn't sound like a good time.
Kiran Krishan: It's, it's so interesting, right? It's weird. It's like. Okay. Um, it's like 10 pages. It's like a little flip book and you kind of scratch and sniff and you try to identify what that smell [00:34:00] is, and then you score yourself at the end.
Yeah. And depending on how discerning your, your olfactory nose is, um, it gives you a score of what your brain health is.
Dr. Brighten: Mm-hmm.
Kiran Krishan: Right? Because it's showing that if your old factory system is starting to get compromised, it likely means that there's a. Dysfunction that's been moving up from your enteric nervous system now starting to enter the central nervous system.
Mm-hmm. So, so for Parkinson's, it'll likely be gut dysfunction.
Dr. Brighten: Okay.
Kiran Krishan: That drives it.
Dr. Brighten: Interesting.
Kiran Krishan: Yeah.
Dr. Brighten: So let me ask you, if someone's listening to this right now and they're like, okay. Need to rebuild my skin microbiome. Where would someone start?
Kiran Krishan: Yeah. I would say start by trying to clean up your personal care products.
Mm. Right. As much as you can. And, and it's, it's hard because there's not a lot available out there, and I don't want people to go get overwhelmed by things and go, oh my God, I gotta throw out my whole medicine cabinet and start over. I would pick one thing. Right? So pick a lotion. Try to find the, and what are people
Dr. Brighten: looking for?
Like what are things that you're [00:35:00] like, absolutely avoid this in skincare products.
Kiran Krishan: Yeah. So when you find things like parabens. Mm-hmm. Right. Um, and then phthalates, parabens, um, you know, you, you see sodium benzoate, um, there's potassium benzoate as well. So these are all the. Preservatives and um, the antimicrobials and antifungals that are found in there.
Dr. Brighten: And these are things that dermatologists actually recommend to people.
Kiran Krishan: Yeah.
Dr. Brighten: So why do dermatologists not understand, understand the skin microbiome?
Kiran Krishan: They're probably like 10 years behind on anything microbiome. Yeah. It's no different than how gastros don't really understand the gut microbiome. Still.
Narrator: Mm-hmm.
Kiran Krishan: Right. It doesn't fall within their scope of work, right? Mm-hmm. So there are very few dermatologists in the country. We know that there's only something like 3000. Um, and, and the vast majority of dermatologists do really well when they do procedures right? So they become very procedure oriented.
And so the person in the dermatology office that's [00:36:00] often managing. Day to day skin health is gonna be the PA or the np, the the physician assistant or the nurse practitioner. Right. And so when I start talking to physician's assistants and nurse practitioners, they start to get it. You see a lot more NPS there.
Mm-hmm. Who are working in dermatology clinics 'cause they're trying to understand the impact of the skin microbiome and they're trying to like recommend cleaner and better. Products to their patients.
Dr. Brighten: Okay?
Kiran Krishan: Right. So, so if it's really complicated and, and, and, um, there's lots of chemical names on there that you don't understand or you can't even read, it's probably not good for you.
Here's another thing, chat. GPT does an amazing job nowadays, right? Take a picture of the ingredient list right in, in chat. If anyone who uses chat, take a picture of the ingredient list and ask chat, GPD if any of these ingredients have been shown to harm this. Skin or the skin microbiome. Mm-hmm. And it'll pull up studies.
Right.
Dr. Brighten: But always. Sure. Yes.
Kiran Krishan: Okay. Make sure no hallucination. So I would say. Start with the [00:37:00] moisturizer. Try to get the cleanest version of moisturizer you can find.
Dr. Brighten: Mm-hmm.
Kiran Krishan: The fewer ingredients the better. If you don't have phthalates and parabens and, uh, benzoates and all that in there. Great. Right. You don't need fragrances in your moisturizer.
So if your moisturizer has all these weird artificial smells and all that, you don't need that. Yeah. Right. You don't need bubblegum smelling lotion.
Dr. Brighten: Has there been any studies on how that alters. The, the microbiome.
Kiran Krishan: Yeah. So there are studies on fragrances mm-hmm. And impact on the microbiome because most fragrances are gonna be volatile, um, compounds.
They're gonna be volatile lipid-based compounds. Right. They're aromatic, volatile, lipid-based compounds. Most of those kill bacteria.
Dr. Brighten: Mm-hmm.
Kiran Krishan: They're actually really strong antimicrobials.
Dr. Brighten: Wow.
Kiran Krishan: Um, kinda like essential oils, also very strong antimicrobials. Mm-hmm. Um, so you also don't want to douse yourself with too many essential oils that, that I see some people doing.
Um. So I would say, so to answer your question about how do you go about starting to fix your skin microbiome. I would say start to clean up your personal care [00:38:00] products. You know, pick a lotion, pick you know, makeup. That's the cleanest that you can find. Uh, pick a, a, a soap or you know, and so on. That's the cleanest that you can find.
Right? Do your best with it. Don't stress, the stress is gonna cause breakout. So don't cause, don't cause yourself stress.
Dr. Brighten: Cortisol will also age your,
Kiran Krishan: is faster it, so it'll, yes, it really does. And so don't stress about it. Do your best. Then the other part of it is as much as you can throughout the day.
Have your skin as natural as possible, meaning it's clean, all the stuff has come off the makeup and everything is off, and then just let your skin be, right. Mm-hmm. And then if you can go out in the natural environment, like go for a walk or a hike or go, you know, in a, in the woods or wherever you may want to go, which is a natural environment with bare raw skin.
Mm-hmm. Right? Because there are lots of transient microbes in the environment. That jump on your skin and they can actually modulate your skin in a dramatic way. I developed a, a serum called siv, [00:39:00] SIV, which is a spore based serum for the skin. Mm-hmm. And we've done a couple of different studies on it, and we see a dramatic improvement on inflammatory conditions in the skin and the microbiome of the skin.
And in, in dermatitis, we're seeing as. Significant improvement in dermatitis and barrier function in the skin because we're adding the spores, which are transient organisms onto the skin.
Dr. Brighten: Mm-hmm.
Kiran Krishan: They get on the skin. They don't live there forever. They hop off in like a day, but when they're on there, they modulate the immune response and they can shift the resident microbes on the skin as well.
Very similar to what a probiotic may do in the gut. Right. So the most natural thing for your skin is interacting with nature. Mm-hmm. Right. That's how we've evolved. Right. Our skin is raw, we're getting dirt on it. We're getting. Sand and dust and all that stuff in a natural environment on it. So we've developed this me mechanism where by which transient microbes hop on, they effectuate certain processes that are reparative, that modulate inflammation, that increase the growth of the resident microbes, and then they hop off.[00:40:00]
Right. So that is one of the most important things you can do for your skin. Get some natural exposure.
Dr. Brighten: If someone is struggling right now with acne, psoriasis, eczema, like they're having skin dysfunction, they're listening to this, let's say they wanna start fresh and new Monday morning. Yeah. What's one thing they could do to start shifting that?
Kiran Krishan: So, dermatitis, there's a couple of things I would do. Um, number one, I would, I would. Clean the areas where you have lesions, right? So most people have dermatitis, which, uh, which is a form which is eczema. You don't have it all over your body. You have leg lesions, usually in the folds of your arms, right in the on, on the other side of your elbows and the back of the legs, the back of the knees, and so on.
If you have a region of your skin where you don't have eczema, what you want to do is clean that region where you do have an eczema, uh, uh, lesion, and then you take a cotton swab with a little bit of water on it mm-hmm. And maybe a, a tinge of oil. And then you, you swab healthy areas of. [00:41:00] Skin and you transfer that and you swab the lesion areas of your skin.
Do that two or three times a day throughout the day after you clean your skin.
Dr. Brighten: Mm-hmm.
Kiran Krishan: I swear there have been so many people that I've recommended this to that have said that they've seen dramatic improvements on the lesions because you're shifting. The microbiome of that part of your skin, right? From your own bugs and the healthy part of your skin.
So that's a simple thing that people can do. Uh, the second part of it is anything that's gonna dry the skin is gonna make your dermatitis worse. Mm-hmm. It's gonna make your eczema worse. Anything that's gonna increase inflammation. So, you know, from a, from a, uh, lotion perspective, CeraVe has some good studies on, it's a topical ceramide.
Synthetic ceramide, but it seems to work right. Uh, but I would also use some oils on there. You know, I would use like an olive oil on there to maintain the moisture on the skin in the area of the lesion.
Dr. Brighten: People have olive oil, avocado oil, and coconut oil in their kitchen. Yeah. What's the best one to choose and what one should you avoid?
Kiran Krishan: I would avoid the [00:42:00] coconut.
Dr. Brighten: Because
Kiran Krishan: the coconut is, has strong antimicrobial. So now in India, I grew up in India, we use coconut oil and everything, and our skin, our hair, everything, right? Mm-hmm. Uh, but, but for most Western people, I wouldn't necessarily use it because I think it'll have a more detrimental effect on the skin.
Mm-hmm. Uh, but olive oil, really great for the skin. Avocado would be number choice number two, coconut would be number three. Mm-hmm. Um, and then, and then the autologous transfer. Um, and then the, the, uh, the, the. Probiotic spores actually, because of our studies on eczema, has a huge impact on changing the skin microbiome and improving the skin as well.
Now psoriasis, you can do some of those same things on the topical side, but with psoriasis, because there's an autoimmune component, you really need to fix your gut. As well, right? Because we both know a dysfunctional leaky gut is driving autoimmune responses throughout the body. There's this, the chronic low grade inflammation aspect of it.
There's the lack of those treg cells, those regulatory T cells. So we need to improve the, the gut [00:43:00] health, which means that we want to use fiber, prebiotics, polyphenols, probiotics that are well tested and and researched, like. The MegaSpore and other, you know, research probiotics. So I would absolutely focus on the gut in people with psoriasis.
Mm-hmm. As well. Mm-hmm.
Dr. Brighten: Well, thank you so much for your time today. I could talk to you forever. We've been friends, what were we saying? It's like 15 years or something like that. It's like, it's
Kiran Krishan: 2012 or 2013.
Dr. Brighten: Yeah.
Kiran Krishan: Yeah.
Dr. Brighten: It's been, yeah, yeah,
Kiran Krishan: yeah. You were living in Oregon or somewhere at the
Dr. Brighten: time,
Kiran Krishan: right? I, yeah.
Dr. Brighten: I remember the first time I met you at a, at a nutrition conference. Yeah. And I walked up and introduced myself, and you were like, I know who you are. And I was, well, I know who you are.
Kiran Krishan: Let's be friends. Let's, let's go to dinner. Yes. I'm
Dr. Brighten: so glad we finally recorded a podcast together. I'm so
Kiran Krishan: excited to be able to do this with
Dr. Brighten: everyone.
Kiran Krishan: Thank you so much. Thank you so much for having me.
Dr. Brighten: Thank you so much for joining the conversation. If you could like, subscribe or leave a review, it helps me so much in getting this information out to everyone who [00:44:00] needs it. If you enjoyed this conversation, then I definitely want you to check out this.


